“I thought it would be good to speak with people who might be able to educate the community about COVID-19 and the vaccine,” says Carey Whitfield, of the NAACP.
Editor’s note: This story is part of Southwest Michigan Second Wave’s On the Ground Battle Creek series.
Carey Whitfield will listen politely to the reasons some in Battle Creek’s African American community give him when talking about their hesitancy or refusal to get the COVID-19 vaccination.
He understands that a shot in the arm for them does not carry the positive connotations that it does for others. But, in his role as President of the Battle Creek chapter of the NAACP and as one who survived his own battle with COVID-19, he is focused on providing the city’s minority communities and people of color with facts and the most up-to-date information from experts.
That focus on information took the form of a communitywide ZOOM call on Tuesday evening (Feb. 10, 2021). It featured panelists Bill Mann, president and CEO of Bronson Healthcare; Melissa Bishop-Murphy, Senior Director-Pfizer Government Relations, Founder and Co-chair of Pfizer’s Multicultural Center of Excellence; Dr. William Nettleton, Medical Director of Kalamazoo County Health and Community Services Department and Calhoun County Public Health Department; and Pastor William Wyne, Pastor of Second Missionary Baptist Church.
“People will share with me what’s on their minds,” Whitfield says, “and many people shared with me that they had no interest in taking the vaccine for a multitude of reasons. But I didn’t think they had enough information to make those radical kinds of decisions and I thought a little more education about the subject matter could be quite valuable for them. I thought it would be good to speak with people who might be able to educate the community about COVID-19 and the vaccine.”
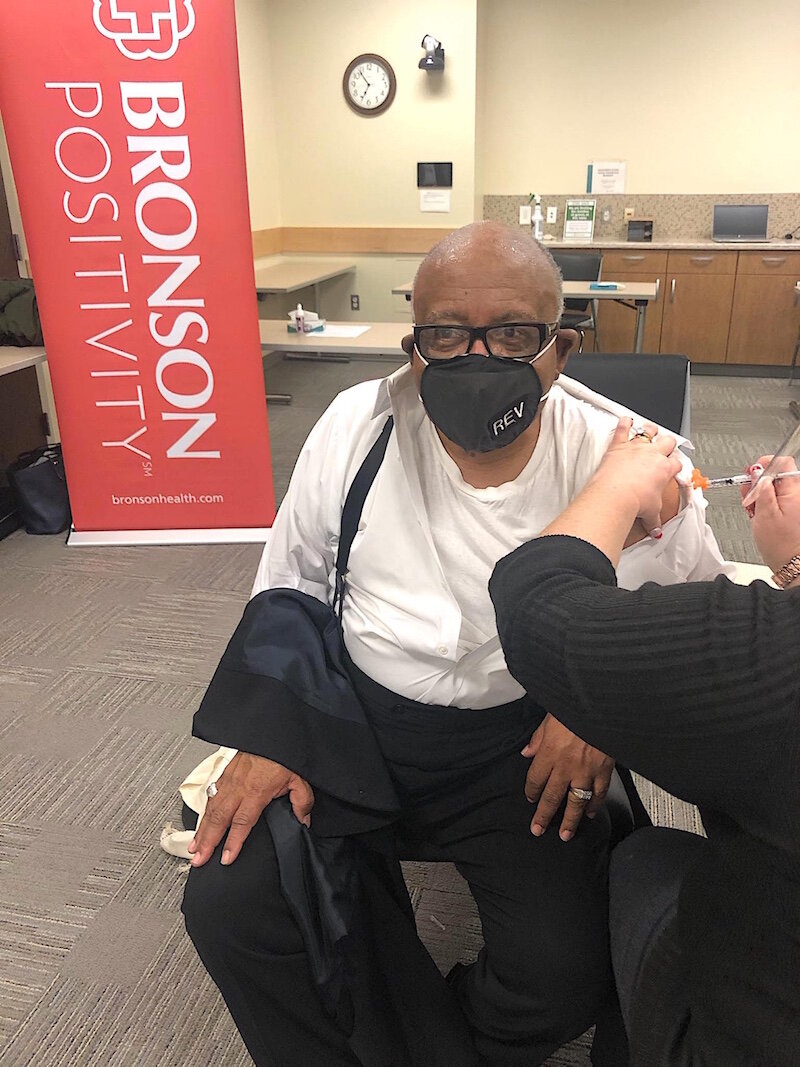
Mann, of Bronson Healthcare, says efforts like this are an important part of overall plans to ensure that as many people as possible are vaccinated. He says he personally has seen the disparities that leaders in the African American community like Whitfield are working to change.
“We recently opened up vaccinations to the general public at four locations,” Mann says. At one of these locations, he says he saw one Black man.
“I literally saw hundreds of patients come through and I saw one Black man. It flowed beautifully, but again I saw one Black man, and I was incredibly devastated. We are looking to partner with others in Battle Creek to ensure that those in vulnerable populations have access to the vaccine.”
The hospital’s Battle Creek vaccination site is operating out of its Fieldstone Center at 165 N. Washington Ave.
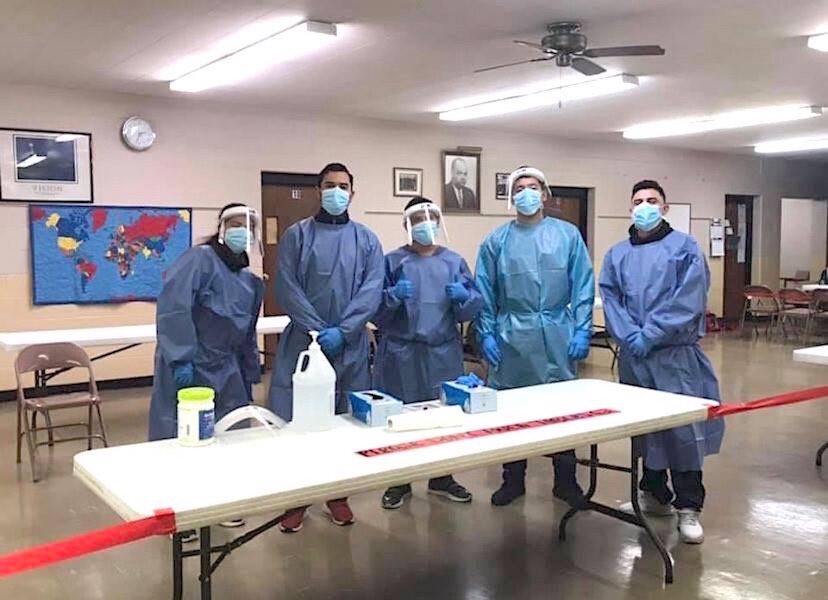
Nettleton says partnering with other organizations such as churches provides the types of opportunities that leaders representing communities of color are looking for. He cited the success of a vaccination clinic held recently at Mt. Zion Church in Kalamazoo.
“When I took the shot I made sure our congregation knew,” Wyne says. “It’s important as an African American church leader that I do everything I can to get information to our churches and make sure people we trust get that information to people.”
Information about the Pfizer vaccine was distributed to members of Wyne’s congregation, Second Missionary Baptist Church.
Suspicion Fueled by Historical Trauma
Like Whitfield, Wyne, who serves in Bronson’s Pastoral Care department, has seen and heard suspicion and fear in the voices of members of the African American community about the vaccine.
Historically, African Americans have not had positive experiences with the medical industry. Examples Whitfield cited included the Tuskegee Syphilis Experiment in which African American men were injected with syphilis virus with no follow-up treatment. The experiment began in 1932 and continued until 1972 under the direction of the U.S. Public Health Service. Wyne also mentioned the forced sterilization of African American women who were among a large group who unknowingly underwent the procedure.
According to an article on the ThoughtCo. website, “Countless numbers of Americans who were poor, mentally ill, from minority backgrounds or otherwise regarded as ‘undesirable’ were sterilized as the eugenics movement gained momentum in the United States. Early 20th century eugenicists believed that measures should be taken to prevent ‘undesirables’ from reproducing so that problems such as poverty and substance abuse would be eliminated in future generations.”
By the 1960s, tens of thousands of Americans were sterilized in state-run eugenics programs, according to investigative reporters for NBC News. North Carolina was one of 31 states to adopt such a program.
“Between 1929 and 1974 in North Carolina, 7,600 people were sterilized. Out of those sterilized, 85% were women and girls, while 40% were people of color (most of whom were Black). The eugenics program was eliminated in 1977 but legislation permitting involuntary sterilization of residents remained on the books until 2003.”
These are among the many reasons why African Americans harbor suspicions about scientists and vaccines, according to a Jan. 21 article in the Chicago Sun-Times. The article cited a survey by the Kaiser Family Foundation which found that nearly one-half (48%) of Blacks and over one-third (38%) of Latinos were not confident that their needs had been taken into account in the development of the vaccines.
“We know our history, and we understand from where this hesitancy comes,” said Dr. Kizzmekia Corbett, the African-American viral immunologist who led the National Institutes of Allergy and Infectious Diseases team that performed the scientific miracle of developing and testing the Moderna vaccine in record time.
“On the one hand, we are the communities most plagued by the pandemic. On the other hand, we are communities least likely to get vaccinated.”
In addition to these suspicions fueled by historical trauma, Wyne says he has fielded questions about the safety and efficacy of a vaccine that was created in nine months versus the normal eight- to nine-year timeframe.
Bishop-Murphy, who is based in Atlanta, says Pfizer routinely partners with national organizations like the NAACP to make sure that the pharmaceutical company’s clinical trials are diverse so that communities are reassured that cures work for black and brown communities. With respect to the COVID-19 vaccine, she says the company is working with community-based allies and addressing vaccine confidence.
The Pfizer vaccine, she says, went through rigorous clinical trial processes.
“Even though it seems like it happened so quickly, over 46,000 people participated worldwide, 30 percent were Black and Brown and 10 percent were African American. We were able to do a lot of the processes in parallel. We went at it as a risk. We assumed the cost of failure and we did not accept any monies from corporations with Operation Warp Speed.”
Pfizer, she says, “worked hand-in-hand” with the FDA, which required 60 days of data from the second dose of the vaccine because of side effects.
The company was granted Emergency Use Authorization, which gives the FDA the ability to fast-track the research and approval process. Bishop-Murphy says the norm is two-year clinical trials, but the nature of the Emergency Use Authorization is that no other alternative because there’s a pandemic.
“We understand there are concerns, but the FDA reviewed the clinical trials and there were safeguards built-in, in addition to the CDC, which also reviewed our clinical trial data. We have done everything we could to make the trials diverse so we know the vaccine works with Black and Brown communities. We want to arm everybody — each one, teach one — about the safety and efficacy of the vaccine.”
These teaching moments need to be expanded to include information about the virus and the vaccine in different languages, says Isabel Sanhou, a Community Health worker who was among the meeting’s 42 participants.
She says the fears expressed by many of her clients are compounded by their inability to understand the scientific jargon so often used in informational pieces.
As a healthcare professional, she says, “I can understand some of it, but if I have a client who doesn’t speak English or understand the terminology, they’re lost. I cannot explain all of these big terms to someone who has not finished high school or doesn’t understand the language.”
This prompted Shirley Tuggle, a retired nurse and community volunteer who was also in the meeting, to ask if Pfizer’s statements about the vaccine could be printed in other languages for distribution throughout the community. Bishop-Murphy says these materials already exist and she would be sending them on to Whitfield.
In addition to printed information, Calhoun County Commissioner Kathy Sue Vette shared with other participants that Burmese and Latinx interpreters have been made available at different vaccine clinics she has volunteered with.
“I understand that it’s quite a process to get seniors of any ethnic background signed up, but once they get there, it’s an amazing and efficient process,” Vette says.
Equitable Access
However, that process is only as good as the number of doses of the vaccine that are available to residents of Calhoun County. During a vaccination clinic on Saturday managed by the Calhoun County Public Health Department, officials were hoping to vaccinate about 900 people, in the 65 and older category. People were getting through with a high degree of efficiency and minimal, if any, wait times, according to a volunteer at the clinic.
This was not the experience that Calhoun County Commissioner Rochelle Hatcher had on Tuesday, the same day as the ZOOM meeting she attended. Hatcher says her mother who lives in Texas and is 82-years-old and has medical issues including COPD and Type-2 diabetes has yet to get a confirmed appointment time or site. She says she spent about five hours trying to get a resolution.
“If she had to be on the computer doing what I had to do today, it would have been very frustrating for her,” Hatcher says.
Bishop-Murphy says Pfizer initially contracted with the U.S. Government for 100 million doses and subsequently contracted with the Biden Administration for 100 million additional doses to be delivered no later than July of this year. She says there is an option to purchase an additional 400 million doses.
State governments, she says, determine how many doses they want each week.
“Pfizer direct-ships to whatever location the government says,” Bishop-Murphy says. “It seems to me that this is something the NAACP could be advocating for with the Public Health department. Every state is different and it depends on who’s running the health department. I would say it’s a situation that needs to be brought to a higher level of attention. It involves advocacy and the education of the government. Some best practices need to be looked at that can be shared with other departments of Public Health.”
Whitfield says he’d like to create vaccination sites in the county’s Black communities to encourage people to get the vaccine but acknowledges that this can’t be done unless there’s an adequate supply.
“We at the local level are just as frustrated as you folks are about the vaccine distribution. It’s challenging to plan ahead when the predictability about the supply is not there,” Nettleton says.
Mann agreed, saying that, “We want to make sure we’ve got enough to give people their second dose. The dose distribution was 50/50 between health departments and health systems. It is now 70 percent to health departments and 30 percent to health systems.”
Locally, public health officials and those who lead senior health organizations have continued to ask for patience as they work through a list of more than 25,000 individuals in Calhoun County who are 65 or older and eligible for the vaccine.
Carla Reynolds, a Battle Creek City Commissioner asked if there is a timeframe to get this done.
“That’s the million-dollar question,” Nettleton says. “We have those who are 65 and older and there’s this whole other category of frontline essential worker. That’s a very large number of people. This is when the partnership between local health systems and public health is beneficial. You can identify people by age and health conditions.”
This prompted Hatcher to ask if 65 is the magic number and whether a resident who is not 65 but who has pre-existing conditions is allowed to receive the vaccine.
Nettleton says this brings additional and necessary questions into the conversation such as: How are these decisions made and what are the ethics around vaccine allocation? How do we deal with multiple diseases and keep people from dying while maintaining the function of society and the issue of equity? He says, “We acknowledge that there are some groups more affected than others by being transparent about how decisions are made.”
Nettleton, who is also an Assistant Professor in WMed’s Department of Family and Community Medicine, says justice is the primary public health ethic among the core ethics he teaches. He says it makes sense to meet people where they’re at and listen to what they’re saying.
“The messenger and partnership are really what matters,” he says. “I look forward to partnerships that come out of this conversation today. This is what community is all about, the importance of partnership and highlighting that this is an issue of justice.”
“There needs to be intentionality on collaborating,” Wyne says. “The clergy, in particular, needs to collaborate together to ensure a pipeline to equity. The African American community and churches can position themselves to be conduits and collaborate and partner to ensure that the vaccine gets disseminated throughout the community.”



















