This article is part of Overloaded and (Often) Unpaid, a joint solutions journalism project on caregiving and mental wellness between the Southwest Michigan Journalism Collaborative and the New York and Michigan Solutions Journalism Collaborative, a partnership of news and community organizations dedicated to rigorous and compelling reporting about successful responses to social problems. The groups are supported by the Solutions Journalism Network.
When our body or mind, for one reason or another, fails us — these are the people who step in to help. Professional caregivers are the front-line heroes who nurse us back to health, who hold our hands when we are alone or hurt, who administer medicine to heal us, and who help us up when we fall.
But who helps caregivers when they are in need?
Caregiver burnout has been a growing problem, especially since the COVID-19 pandemic when hospitals, skilled nursing facilities, and senior communities have been overwhelmed.
There is sometimes an assumption that professional caregivers can handle the stress. After all, it’s their job.
Yet there is a cost for not addressing the health of paid caregivers. The Centers for Disease Control and Prevention list the negative effects of poor mental health among employees: reduced job performance and productivity; a lack of engagement with one’s work; a decrease in communication with coworkers; and poor physical capability and daily functioning in the workplace.
Keeping caregivers healthy in mind and body is important for them as well as for those who depend upon them.
That’s why employer-based support is so important.
According to Statista, a 2021 survey, nurses said the most common reason they planned to leave their job was that work had negatively affected their health and well-being. The second most common reason was insufficient staffing. In 2020, the average turnover rate for registered nurses across the United States was 18.7 percent.
In the hallways of hospitals
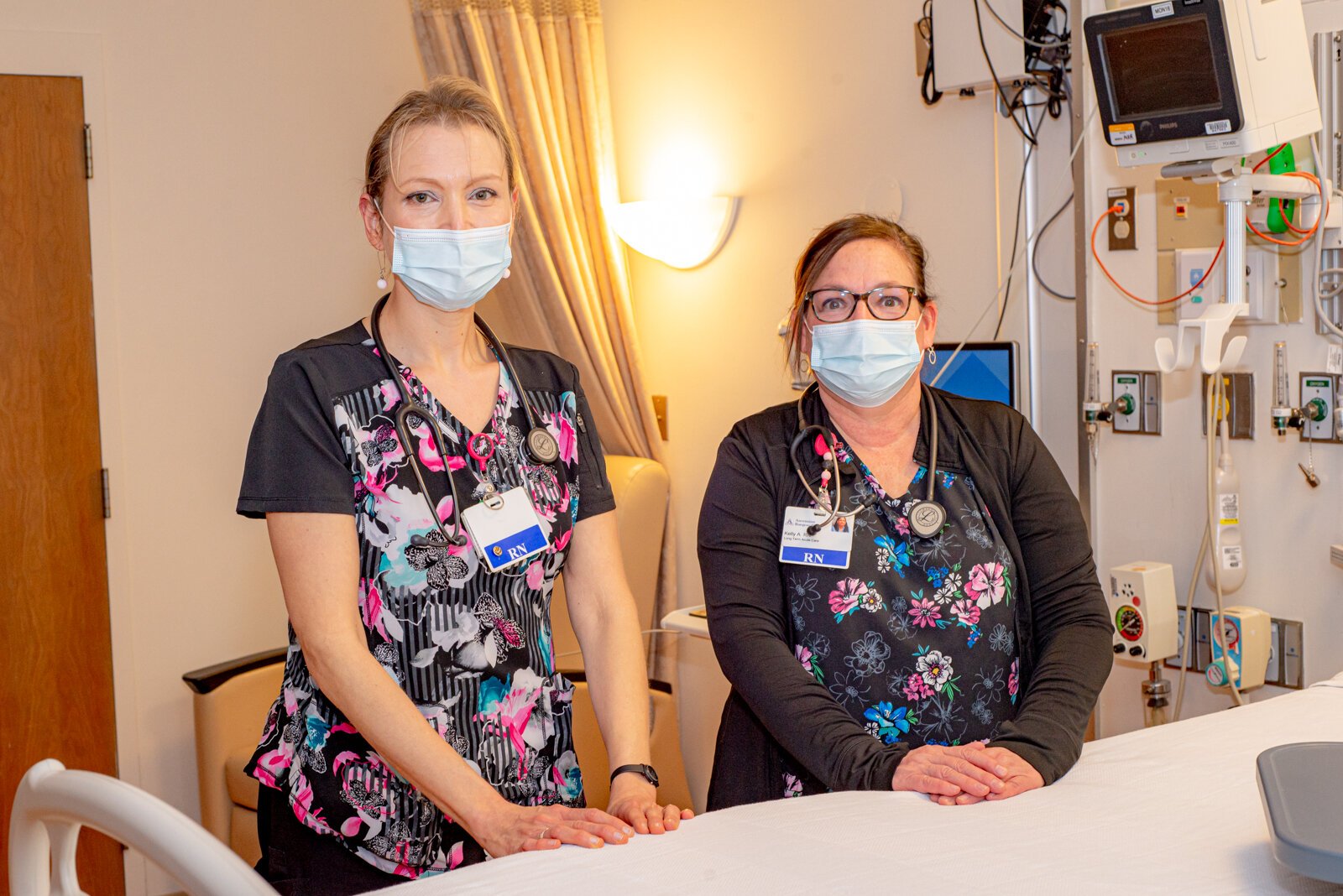
Angela McIntyre and Kelly Asselmeier are registered nurses at Ascension Borgess-Pipp Hospital, a long-term acute, special needs and emergency care facility in Plainwell, Michigan. McIntyre has worked in nursing for almost four years; Asselmeier for 12 years. Their usual shift is 12.5 hours with a 3- to 4-day work week.
“In nursing, you see the whole gamut,” McIntyre said. “Many of our patients are on ventilators, many are critically ill. You have to think with your head and your heart at the same time. For me, when I went into this, I wanted to be there for people in their hardest moments, but sometimes they die, and that can take its toll.”
“During Covid, we weren’t always able to get to everyone in time, and that was horrible,” Asselmeier said. “It could be overwhelming … We love our work, but that was hard.”
That level of stress over time can lead to burnout. Burnout can lead to staff turnover. Health care employers know the importance of taking care of their workers. At Ascension hospitals in southwest Michigan, employees have access to MyCare, a website that connects health care workers to resources such as online therapy, virtual or in-person spiritual care, a list of crisis hotlines for substance abuse, suicide, and more.
“I like to think of MyCare as something like a spare tire,” McIntyre said. “You know where it’s at, where it’s located, but you don’t want to be at the point where you need it. But sometimes, as nurses, we do need to go to others for support. It’s a wealth of resources.”
McIntyre participates in virtual therapy offered on MyCare.
“I do go to therapy each week, which Ascension does cover,” she said. “I do it on video, right from my couch with my cup of coffee. My therapist is cool because she understands caregiver burnout.”
In the day-to-day, both nurses look first to their direct management and coworkers for support. Incentive pay for the extra hours and holidays can also keep nurses motivated.
“Appreciation from our own team means the most,” Asselmeier said. “And we get that from our patients, too. They are the reason we are there.”
Debriefing meetings after a patient dies is a valuable check-in on caregivers’ mental health needs. Transparency about work issues keeps the team feeling included rather than managed.
Not to be ignored are the small but meaningful shows of appreciation. A recently installed “massage room” at the hospital allows nurses on break to relax in a comfortable leather massage chair under dimmed lights. A quiet space gives nurses an opportunity to defuse stress and meditate. “Little things matter,” McIntyre said. “All of these things matter.”
Ascension offers tuition reimbursement — a benefit McIntyre used to complete her bachelor’s degree in nursing.
Caring for seniors
Friendship Village in the greater Kalamazoo area is an example of what works in preventing caregiver burnout. The longevity of their staffers’ employment indicates the senior community that spans care from independent living to memory care, is doing something right.
Reagan Rhoderick, director of resident services; Stephanie Edwards, director of human resources, Ashley Jamieson, director of nursing for Woodside Assisted Living at Friendship Village, and Diana Duncan, director of sales and marketing, came together at Friendship Village to talk about the support systems available to their health care workers.
“We were not immune to staffing struggles during the Covid pandemic,” Jamieson said. “But perhaps we did not experience it as badly here as those at hospitals and other facilities. In great part, I believe, that is because of the relationships we develop. … Our staff has a lot of longevity because of that kind of attention.”
Maintaining a ratio of 1 nurse to 10 residents in assisted living, around the clock, helps to keep staff from becoming overwhelmed. Caregivers who are not RNs have nurses to support them as needed.
“During Covid, we locked our doors for a time to prevent contagion, and when there was a breakout in November 2020, those were 45 days of pure hell,” Jamieson said. “We lost 23 residents, five in our worst day, and 40 residents tested positive. Our staff went into autopilot, working 60 and more hours a week. We shared staff across the facility, wherever the need was greatest. But if anything good came from that, it was that our people bonded and became closer than ever. It was combat nursing.”
Caregivers understand they have the permission and flexibility to care for themselves.
“We include empathy training in our orientation for new hires,” said Duncan. “Our staff is explicitly told that they have permission to walk away if they are feeling overwhelmed — let someone else step in. Walk away if you are frustrated. Walk away if you need to take a breather.”
Friendship Village provides its caregivers access to professional assistance in addition to its informal support network.
“We also offer a number of employee assistance programs for employees and their family members,” said Edwards. “Our counseling program offers five visits per episode or work situation where a person feels they need to talk. And legal help is available, or referral to a specialist.”
To show staff members they are valued, Friendship Village recognizes caregivers with gifts and awards.
“There are a number of awards for caregivers,” Duncan said. “There’s an award called Extraordinary Impressions to recognize staff, and each month residents and caregivers nominate someone for the GEM Award.
Caregivers win a $500 experience once a year, to spend however they wish, and we put their photo on the wall and a special parking spot. There’s a $50 gift card, too.”
Friendship Village also encourages employee professional growth by offering tuition reimbursement for full-time team members, as well as conferences and training opportunities.
“We are in the business of people,” Duncan said. “It’s not just one solution. It’s a matter of a multidimensional approach to caregiver mental health and wellness. We take care of our own.”
Keeping caregivers healthy and happy
Successful support programs to ensure caregiver health include access to professional counseling and therapy, recognition and awards, open-door policies to leadership, time and space to decompress, and team bonding. It’s about providing a whole package of robust supports.
The 2017 study, titled “Nurses’ Burnout: The Influence of Leader Empowering Behaviors, Work Conditions, and Demographic Traits” determined in their conclusion these significant factors:
“The results of this study highlight the importance of the leadership role in creating a positive work environment by enhancing the meaningfulness of work, enabling employees to participate in decisions related to their work, expressing confidence in employees’ abilities to perform at a high level, facilitating goal attainment, and providing autonomy. In addition, attracting more nurses to the profession may be achieved by improving nurses’ work conditions, which may enable nurses to remain in the profession longer. These approaches are expected to decrease nurse burnout and consequently contribute to ongoing efforts to reduce the nursing shortage and improve the quality of care provided.”
For those not able to access support systems at the workplace, Courage to Caregivers’ website, offers support to all caregivers, whether professional or family members. They provide one-to-one caregiver peer support, meditation classes, support groups, assistance in creating self-care plans, and SMART (specific, measurable, achievable, realistic, and time-sensitive) goals and educational resources.
Resources